
The Malaria Racketeers of Africa: Counterfeit Nets and Stolen Hospital Supplies
Why it matters:
- The diversion of aid meant to combat malaria in Africa has led to a shadow economy profiting from counterfeit and stolen medical supplies.
- The theft and resale of life-saving commodities not only drain financial resources but also result in deadly consequences for vulnerable populations.
On March 11, 2025, inside a sweltering warehouse in Kano, Nigeria, enforcement agents from the National Agency for Food and Drug Administration and Control (NAFDAC) uncovered a lethal cache. They seized 17,280 bottles of a pediatric suspension labeled “Cikatem.” To the untrained eye, these bottles contained Artemether Lumefantrine, the gold standard treatment for malaria in children. In reality, the liquid was a useless concoction, missing the vital active ingredients needed to kill the parasite. These thousands of bottles were not merely counterfeit products; they were stolen potential, diverted resources, and, ultimately, death sentences for the children who would ingest them.
This seizure represents the visible tip of a submerged iceberg. While the global health community celebrates progress, a shadow economy has taken root within the supply chains of international aid. This is the silent crisis of the diverted aid epidemic. Between 2020 and 2025, as donor funding plateaued and the biological threat of the malaria parasite evolved, criminal syndicates and corrupt officials turned life saving commodities into illicit profit.
The Scale of the Loss
The stakes of these Malaria Racketeers in Africa could be further higher. The World Malaria Report released in late 2025 painted a grim picture: 610,000 lives lost to the disease in 2024 alone. The report estimated 282 million new cases globally, with the vast majority concentrated in Africa. Yet, as the death toll climbed, the financial arsenal to fight it weakened. The gap between needed funds and available resources widened significantly. In 2024, the world had only $3.9 billion available for malaria control, far short of the $9.3 billion target set by global strategies.
Data Point: A February 2025 audit by the USAID Office of Inspector General revealed that despite investing over $9 billion since 2005, the agency struggles to track commodities effectively once they enter partner countries. The audit highlighted that theft, transport, and resale of bed nets and pharmaceuticals remain persistent threats to program integrity.
Every dollar lost to theft in this environment is not just a financial statistic; it is a calculation of mortality. When a warehouse manager diverts a pallet of nets to a local market, or when a pharmacist sells donated ACTs out the back door, the deficit is paid in human life.
Nets into Cash
The mosquito net remains the most iconic symbol of the fight against malaria. Yet it has also become a currency. A 2023 investigation by the Global Fund Office of the Inspector General identified multiple instances of product diversion. in one glaring case, an implementer staff member with warehouse access stole 5,200 insecticide treated nets. These nets, designed to protect sleeping families from the Anopheles mosquito, often resurface in local markets, sold for cash to unsuspecting buyers who should have received them for free. Worse still, many stolen nets are repurposed for fishing, devastating local ecosystems while leaving children exposed to bites at night.
The theft creates a vacuum that counterfeiters are eager to fill. By early 2025, reports surfaced of “fake” nets flooding markets in West Africa. These nets lacked the necessary pyrethroid coating or physical durability to stop mosquitoes, offering a false sense of security that proved fatal.
The Counterfeit Trap
The diversion of genuine medicine opens the door for dangerous fakes. The “Aflotin” scandal of April 2025 exposed this ruthless dynamic. NAFDAC alerted the public to a batch of counterfeit tablets circulating in Nigeria. The packaging mimicked legitimate donor funded stock, but the pills were chalk. This creates a double tragedy: the patient dies from untreated malaria, and the community loses faith in the medical system. When genuine drugs are stolen and sold at a premium, the poor are forced toward these cheaper, deadly alternatives.
As we delve deeper into this investigation, we will expose the mechanics of this racket. We will trace the path of a stolen box of medicine from a dock in Mombasa or Lagos to a street stall hundreds of miles away. We will look at how paperwork is forged, how inventory counts are manipulated, and how the very people entrusted with delivering hope are sometimes the ones snatching it away. This is not just corruption; it is a crime against humanity, executed in the shadows of warehouses and bureaucratic offices.
Anatomy of the Supply Chain: From Global Manufacturers to National Ports
The journey of a mosquito net begins in the industrial weaving districts of East Asia, primarily Vietnam, China, and India. These massive production hubs churn out millions of nets annually, bound for the most vulnerable communities in Africa. Yet for criminal syndicates, this global logistics flow represents a lucrative opportunity for diversion. The modern supply chain, despite its digital tracking systems and audits, remains porous. Between the factory loading dock and the national port of entry, legitimate humanitarian aid is systematically bled into the black market.
Data released in late 2025 paints a stark picture of this leakage. In December 2025, the World Health Organization reported a rise in malaria cases to 282 million globally for the year 2024. A significant factor in this resurgence is the failure of commodities to reach their intended users. The supply chain fractures not at the manufacturing level, where oversight is relatively strict, but at the points of handover: the shipping containers, the customs clearing houses, and the intermediate warehouses.
The Pivot Point: Diversion at the Port
The most critical vulnerability lies at the port of entry. Here, criminal networks exploit bureaucratic opacity. A prime example surfaced in a March 2025 investigation by the USAID Office of Inspector General. The inquiry exposed a sophisticated theft ring involving nets intended for Guinea. Instead of reaching families in Conakry or rural Guinean districts, these supplies were diverted across the border to Bamako, Mali. The scale was immense. Investigators tracked down 200,000 nets worth approximately 386,000 dollars.
This incident reveals the anatomy of the crime. The thieves did not merely steal the goods; they reintegrated them into the commercial sector. The stolen nets were found being repackaged. Racketeers stripped the humanitarian branding, often marked “Not for Sale,” and wrapped the products in counterfeit packaging that mimicked commercial brands. This laundering process allows stolen aid to be sold openly in local markets, funding the very criminal enterprises that destabilize the region.
The Circular Theft Mechanism
The sophistication of these schemes has evolved beyond simple looting. The 2025 Mali investigation uncovered a “circular theft” mechanism. A local company had won a Ministry of Health tender to replace borrowed stock. To fulfill this contract, the company effectively sold stolen donor nets back to the donor. They delivered 117,000 nets to a warehouse, claiming they were new procurements. In reality, these were the very same nets diverted from the Guinea shipment. This circular flow—stealing aid to sell it back to aid agencies—represents a chilling efficiency in modern supply chain fraud.
Counterfeits and the Market for Fakes
When genuine goods are stolen, they create a vacuum often filled by dangerous fakes. The Global Fund reported in 2024 that complaints regarding product theft and diversion had risen by 95 percent since 2020. This surge correlates with an influx of inferior quality nets and antimalarial drugs. Reports from 2023 indicated that nearly one third of antimalarial medicines circulating in parts of the African region were either falsified or substandard. These counterfeits look identical to the real products but lack the necessary active pharmaceutical ingredients or insecticide treatments.
The impact is lethal. As genuine supplies disappear into the black market, health ministries are left distributing ghost inventory or fighting outbreaks with ineffective tools. The 2025 World Malaria Report highlighted that the funding gap had widened to over 5 billion dollars. Every net stolen and every container diverted widens this deficit, transforming the supply chain from a lifeline into a mechanism for profit extraction.
The Vanishing Point: Theft and Corruption at Customs and Entry
The journey of a mosquito net from a factory in Asia to a rural clinic in Africa is fraught with peril, but nowhere is the danger greater than at the port of entry. This is the vanishing point. Here, amid the chaos of shipping containers and the thick fog of bureaucracy, life saving commodities frequently disappear into the hands of criminal syndicates. Between 2020 and 2025, investigations have revealed that customs clearing processes and initial warehousing are not merely logistical steps but active crime scenes where millions of dollars in malaria supplies are diverted.
The mechanism of theft is often buried under mountains of paperwork. In many documented cases, valid import licenses are cloned or manipulated. A shipment of antimalaria medicine arrives at a bustling port like Lagos or Conakry, is signed for by officials, and then seemingly evaporates. The 2023 Annual Report from the Office of the Inspector General (OIG) of the Global Fund exposed the stark reality of this diversion. The report detailed six specific cases across three countries where health products were stolen or diverted. In one egregious instance, an implementer staff member with authorized access to a warehouse orchestrated the theft of 5,200 insecticide treated nets. These were not lost to clerical error; they were physically removed and funneled into private markets where the poor are forced to pay for what should be free.
This theft is rarely the work of a lone opportunist. It requires collusion. Customs officials, transport coordinators, and warehouse managers form networks that exploit the lack of real time tracking. An audit of Global Fund grants in Guinea, published in December 2024, highlighted how fragile these supply chains remain. The auditors found material stock outs and significant gaps in commodity traceability at the central level. The report noted that a warehouse used for storage was unsuitable for safeguarding these valuable assets. When inventory systems are weak and warehouses are insecure, thousands of doses of Artemisinin based combination therapies can vanish without leaving a digital trace. The 2024 findings indicated that the country faced risks of reduced quality and availability, directly linked to these supply chain fissures.
The scale of the problem is magnified by the value of the commodities. A single container of antimalaria drugs can be worth hundreds of thousands of dollars on the black market. In nations like Malawi, the theft of these drugs has been described as rampant. Reports circulating between 2020 and 2025 suggest that up to 30 percent of medicines in some public supply chains disappear before reaching patients. These stolen goods resurface in private pharmacies or are smuggled across borders to neighboring countries. The losers are the patients in public clinics who are told that the pharmacy is empty.

Malaria Racketeers Infographic
Efforts to tighten security often push the corruption deeper into the system. When physical inspections increase, racketeers switch to phantom shipments. They create paper trails for goods that never existed or were diverted before reaching the port. The United States Agency for International Development (USAID) and its OIG have maintained active investigations into these frauds throughout the 2022 and 2023 fiscal years. Their oversight has uncovered schemes where commodities provided by the President’s Malaria Initiative were transported and resold for profit. These are not victimless crimes. Every stolen net and every diverted box of medicine represents a child left unprotected against a deadly parasite.
The data from 2020 to 2025 paints a grim picture of systemic leakage. While international donors pour billions into procurement, the vanishing point at customs remains a critical vulnerability. Without rigorous enforcement, digitized tracking that bypasses human interference, and harsh penalties for corrupt officials, the ports will continue to function as sieves. The fight against malaria is not just a medical battle; it is a logistical war against organized theft.
Warehouse Leaks: Inventory Fraud within National Medical Stores
The most sophisticated thefts do not happen at gunpoint on a dusty highway. They happen quietly, under the fluorescent lights of state owned warehouses, buried within spreadsheets and falsified audits.
Between 2020 and 2025, a new pattern of “inventory fraud” emerged across central medical stores in Africa. Criminal syndicates, often involving senior warehouse managers, have moved beyond simple pilferage. They now employ complex accounting schemes to make millions of dollars worth of antimalarial drugs and nets vanish from official records before they even leave the loading dock.
The “Loan Repayment” Scheme
A striking example of this administrative sleight of hand was exposed in a March 2025 investigation involving USAID supplies in West Africa. The case revealed a circular theft economy that would impress any forensic accountant. The Ministry of Health in Mali had borrowed 200,000 mosquito nets from USAID to cover a stock rupture during a routine distribution campaign. To repay this “loan,” the Ministry hired a private contractor to procure replacement nets.
The contractor did deliver 117,000 nets to the USAID warehouse in Bamako. However, investigators discovered these were not new commercial goods. They were the very same nets that donors had purchased for distribution in neighboring Guinea and Sierra Leone. The syndicate had diverted supplies intended for families in Conakry and Freetown, smuggled them across the border into Mali, and repackaged them. They then sold these stolen goods back to the donor to settle the government debt. The fraud effectively charged the United States government twice for the same humanitarian aid while leaving vulnerable populations in Guinea without protection.
The 30 Percent Leak
In Malawi, the situation within the Central Medical Stores Trust (CMST) illustrates the sheer scale of the problem. Government data from 2024 indicates that the state loses approximately 30 percent of all procured medicines to theft. This is not accidental loss; it is systemic extraction.
Audits reveal that the theft occurs primarily during the procurement and ordering stages, long before the trucks start their engines. Corrupt officials manipulate stock cards to show that drugs were dispatched to rural clinics that never requested them. In other instances, “ghost” health centers—facilities that exist only on paper—are listed as recipients of large shipments of Coartem. The physical inventory is sold to private pharmacies where a single course of stolen antimalarial treatment sells for a premium.
“It is no longer about government not providing medicines, but more about unscrupulous actors robbing families of hope,” stated a Ugandan official in late 2025, following the arrest of five staff members from the National Medical Stores caught coordinating with hospital workers to divert supplies.
Inside the “Syndicated Corruption”
The term “syndicated corruption” has become common in official reports from Uganda to Nigeria. In October 2025, Ugandan police detained staff from the National Medical Stores (NMS) and the Hoima Regional Referral Hospital. The investigation revealed that NMS employees were not acting alone; they had formed a cartel with hospital administrators. The NMS staff would officially “deliver” the drugs, and hospital staff would sign the proof of delivery documents. In reality, the boxes remained on the truck or were offloaded directly into private vans waiting nearby. The paperwork was perfect; the shelves were empty.
This internal collusion renders standard tracking technology useless. GPS trackers on trucks show the vehicle arrived at the hospital. Digital logs show the inventory was received. But the physical goods enter the black market immediately. In Nigeria, where the House of Representatives launched a probe in late 2025 into the utilization of $4.6 billion in Global Fund and USAID grants, similar discrepancies plagued the supply chain. Despite massive funding, malaria burden remained stubbornly high, a statistical impossibility unless a significant portion of the tools to fight the disease were never actually deployed.
The consequence of these warehouse leaks is measured in lives. When a warehouse manager falsifies a ledger to hide the theft of 50,000 nets, the impact is delayed but deadly. Six months later, during the peak rainy season, a district health officer will open a pallet to find it empty, leaving thousands of children exposed to the bite of the Anopheles mosquito.
Chemical Illusions: Laboratory Analysis of Counterfeit Long Lasting Insecticidal Nets (LLINs)
The most dangerous counterfeit product in the global malaria fight does not always look like a fake. It feels correct to the touch. The mesh size is standard. The polyethylene fibers gleam with the promise of protection. Yet, under the lens of advanced chromatography, these nets reveal themselves as “chemical illusions.” They are physical barriers that lack the invisible chemical shield required to kill mosquitoes. Between 2020 and 2025, laboratory analysis of diverted and substandard nets has exposed a sophisticated trade where visual compliance masks a deadly lack of active pharmaceutical ingredients.
The Tanzania Market Anomaly (2025)
A critical investigation led by researchers in Tanzania and published in 2025 exposed the scale of this deception in commercial markets. While donor funded campaigns distribute verified products, the private retail sector tells a different story. The study found that nearly all commercially available nets in surveyed Tanzanian markets were untreated. These products dominate the retail space, sold to consumers who believe they are purchasing the “gold standard” of malaria prevention.
These nets mimic the appearance of genuine Long Lasting Insecticidal Nets (LLINs) but contain zero active ingredients. A family sleeping under such a net receives only a physical barrier, which is insufficient in areas with high mosquito density. The mosquitoes feed on the arm resting against the mesh or find their way through small tears, surviving to bite again because no insecticide is present to knock them down.
Molecular Deception: The Papua New Guinea Findings
The deception goes deeper than simply missing chemicals. A 2023 study focusing on nets delivered to Papua New Guinea utilized Liquid Chromatography Mass Spectrometry (LC MS) and X Ray Fluorescence (XRF) to analyze insecticide content. The results highlighted a terrifying technological failure in substandard manufacturing.
Researchers discovered that having the correct amount of chemical inside the fiber does not guarantee safety. In several batches of PermaNet 2.0 analyzed during this period, high levels of Deltamethrin were detected, yet the nets failed bioefficacy tests. The insecticide was “locked” inside the polymer matrix due to poor coating technology. It crystallized within the fiber, making it unavailable on the surface to kill the mosquito. To a basic chemical audit, the net passes. To a mosquito, the net is harmless. This “availability gap” allows manufacturers to use cheaper, unstable binding agents while technically meeting the total chemical weight requirements on a datasheet.
Diverted Supplies and Repackaging Fraud
The Global Fund Office of the Inspector General provided data between 2022 and 2023 regarding the diversion of legitimate supplies which fuels the counterfeit market. In Guinea, over 117,000 nets were diverted from a mass distribution campaign. These genuine nets often end up repackaged or mixed with fake stocks in neighboring countries like Mali.
Traffickers strip the original packaging, which contains batch numbers and expiration dates, and place the nets into generic or counterfeited branded bags. This breaks the chain of custody. A 2025 analysis in Kenya showed that as nets age or are repackaged improperly, the Piperonyl Butoxide (PBO) content—a crucial synergist added to overcome resistance—degrades rapidly. The Kenya study revealed that PBO nets lost bioefficacy significantly within 18 months when storage conditions were compromised, a common reality in the black market supply chain.
The Alpha Cypermethrin Deficit
Further chemical profiling in 2024 has focused on nets treating Alpha cypermethrin. In substandard versions found in regions south of the Sahara, the dosing is inconsistent. While WHO specifications demand precise milligrams per square meter, seized samples often show variations of 40 percent or more across a single net. One quadrant of the fabric may be lethal to vectors, while another is benign.
This patchy application creates a training ground for resistance. Mosquitoes contacting the sublethal zones survive the exposure, passing on resistance genes to their offspring. The counterfeit trade is not just failing to kill mosquitoes today; it is breeding the super mosquitoes of tomorrow.
The laboratory evidence from 2020 to 2025 is clear. The enemy is no longer just the mosquito but the net itself. Through total absence of chemicals, unavailable active ingredients, or degraded stock sold as new, these chemical illusions provide a false sense of security that is measured in rising case numbers and stalled eradication efforts.
The Placebo Effect: The Deadly Trade in Fake Artemisinin Combination Therapies
In the humid wards of rural clinics across West Africa, a silent mechanism of murder is taking place. It happens not with a weapon, but with a blister pack. A mother administers a tablet to her feverish child, believing it to be the gold standard cure for malaria. The packaging is glossy, the hologram authentic, and the manufacturer’s stamp precise. Yet, inside the child’s body, nothing happens. The fever spikes. The parasites multiply unchecked. This is the deadly reality of the trade in falsified Artemisinin based Combination Therapies (ACTs), a criminal enterprise that has turned the miracle cure for malaria into a weapon of mass deception.
Between 2020 and 2025, while the world focused its attention on the viral pandemics, a parallel crisis exploded in the tropical belt. The United Nations Office on Drugs and Crime (UNODC) released a harrowing assessment in 2023, estimating that falsified and substandard antimalarials are now linked to nearly 267,000 deaths every year in the region south of the Sahara. This figure represents a hidden genocide, driven by profit margins that rival the narcotics trade but carry a fraction of the risk.
- Annual Deaths: Approximately 267,000 in sub Saharan Africa due to fake antimalarials.
- Market Penetration: 19 to 50 percent of medical products in the Sahel are substandard or falsified.
- Seized Volume: Over 605 tons of illicit medical products seized in West Africa since 2017.
- Economic Cost: Up to $44.7 million spent annually caring for patients treated with useless drugs.
The criminals behind this racket operate with sophisticated impunity. The supply chain for genuine ACTs is infiltrated at multiple points. Investigations reveal that many of these counterfeit products originate from legitimate pharmaceutical hubs in Asia and Europe, diverted from legal channels and repackaged, or are manufactured in illicit clandestine laboratories within the region. A 2023 UNODC report highlighted that as much as 50 percent of the medical products circulating in the Sahel belt could be substandard or falsified. In countries like Burkina Faso and Guinea, the shelves of roadside pharmacies are flooded with these placebo killers.
The danger is twofold. First is the immediate tragedy of therapeutic failure. A patient treated with chalk or starch simply dies from untreated malaria. But the second threat is perhaps more catastrophic for the long term future of global health: drug resistance. Many “fakes” are not entirely devoid of active ingredients; instead, they contain trace amounts of artemisinin. This underdosage is insufficient to kill the parasite but perfect for training it to survive. By exposing the malaria parasite to weak waves of the drug, these criminal syndicates are effectively breeding superbugs that could render our best defenses useless.
The economic toll is equally staggering. The World Health Organization estimates that the region spends millions annually treating people who have already “received” treatment. This creates a vicious cycle of poverty and illness, where families sell assets to buy medicine that fails, only to face higher hospital bills when the disease progresses to a critical stage.
Recent crackdowns have exposed the depth of the rot. In 2022 and 2023, major seizures in Nigeria and Cameroon uncovered warehouses stacked with millions of fake doses. Yet, enforcement remains a challenge. The borders are porous, and the regulators are often outgunned and underfunded. The counterfeiters use state of the art printing technology to replicate security seals, making it nearly impossible for a layperson to distinguish the cure from the poison.
As we move through 2025, the international community faces a stark choice. The continued flow of falsified ACTs is not merely a trade violation; it is a dismantling of the public health infrastructure. Without a coordinated global response involving track and trace technology and stricter supply chain audits, the miracle of artemisinin will be lost, stolen by racketeers who trade human lives for pennies on the dollar.
Street Corner Pharmacies: Tracking Stolen ‘Not For Resale’ Vials
Under the corrugated iron roof of a makeshift stall in Lilongwe market, the heat is oppressive. The vendor, a man in his late forties known locally as “Doctor” Banda, arranges his wares on a wooden table. Between herbal remedies and loose painkillers sit boxes of Artemether Lumefantrine, the gold standard treatment for malaria. The packaging is green and white, unmistakable to those who know the brand Coartem. But there is a telltale scar on the cardboard. A razor blade has been used to scrape away a specific patch of text. If one looks closely at the abrasion, the ghost of the words “NOT FOR RESALE” remains visible. These medicines were paid for by Western taxpayers and intended for free distribution in public clinics. Instead, they are here, selling for a price that forces families to choose between food and survival.
This is the ground zero of a global theft epidemic. Between 2020 and 2025, investigations by the Global Fund and the World Health Organization revealed a systemic diversion of antimalaria commodities that bleeds health systems dry across Sub Saharan Africa. While counterfeit nets garner headlines, the theft of genuine pharmaceutical vials is a more insidious crime, turning humanitarian aid into black market profit.
The Supply Chain Leak
The journey of a stolen vial begins long before it reaches the street corner. In December 2023, the Global Fund suspended two major malaria grants in Mali after auditors uncovered evidence of “misappropriation and unjustified expenditure.” The investigation highlighted a grim reality: the thieves are often on the inside. Warehouse managers, transport drivers, and corrupt hospital administrators form a coordinated ring that diverts stock the moment it arrives in country.
In 2024, the situation in Malawi reached a breaking point. Government data indicated that approximately 30 percent of medicines purchased or donated for the public sector were disappearing. These drugs do not vanish into thin air; they flow into private clinics and street markets. An audit revealed that nearly one in three private pharmacies in the capital stocked drugs bearing the erased “Government of Malawi” or “Global Fund” markings. The sheer scale of this pilferage prompted the World Bank to fund a pilot program in late 2024, embedding electronic tracking devices inside 2,387 medicine boxes to monitor their movements in real time.
The ‘Not For Resale’ Economy
The “Not For Resale” (NFR) stamp is designed to be a protective charm, a legal barrier against commercialization. In practice, it has become a mere inconvenience for racketeers. Organized criminal groups employ teams of “cleaners” whose sole job is to remove these markings. They use acetone to wipe ink from blister packs and scalpels to excise the text from outer cartons.
The 2023 Annual Report from the Office of the Inspector General (OIG) of the Global Fund noted a 24 percent increase in complaints regarding fraud and abuse compared to the previous year. The report detailed specific instances where implementer staff members with access to warehouses diverted thousands of health products. In one egregious case, over 5,000 insecticide treated nets were stolen by a single employee. But the medicines command the highest street value. In a region where malaria claimed 610,000 lives in 2024 alone, a guaranteed cure is a commodity worth stealing.
Consequences of Diversion
The theft of NFR drugs creates a deadly paradox: public hospitals run out of stock, forcing patients to buy stolen public drugs from private vendors. This cycle effectively privatizes aid, stripping the poorest citizens of their right to health care.
“When a mother walks into a free clinic and is told there are no drugs, she walks out to the market and buys the exact same box that should have been on the clinic shelf. She is buying back her own stolen right to life.” — Global Health Audit Report, 2024.
Furthermore, this unregulated street trade fuels drug resistance. Street vendors sell individual blister packs rather than full courses, or they sell expired stock that has been relabeled. Inconsistent dosing contributes to the rise of partial resistance to artemisinin, a threat the WHO flagged as “acute” in its December 2024 World Malaria Report. Confirmed resistance has now been documented in eight African nations, a ticking time bomb that could render current treatments useless.
The Tech Counteroffensive
The response has been slow but is gaining momentum. Beyond the World Bank’s tracking devices, donors are demanding stricter accountability. In 2025, the United States threatened to withhold 50 million dollars in health aid to Zambia after repeated warnings about theft went unheeded. This hardline approach signals a shift in donor strategy: no more blind checks. The Global Fund is now implementing “Spot Checks” and requiring digital inventory systems that are harder to manipulate than paper ledgers.
Yet, for the vendor in Lilongwe, business continues. As long as the demand outstrips the secure supply, the razor blades will keep scraping, and the “Not For Resale” vials will continue to be the most profitable item on the shelf.
The Fishing Syndicate: Industrial Misuse of Nets for Agriculture and Aquaculture
The dawn over Lake Victoria reveals a fleet not of trawlers, but of canoes drifting in silence. These are not standard fishing vessels. They drag behind them a distinct blue or white fabric, shimmering with a chemical sheen. These are not fishing gear. They are life saving tools meant for beds, now repurposed into instruments of ecological extraction. This is the visible face of the fishing syndicate, an organized misuse of malaria prevention supplies that has turned humanitarian aid into a driver of aquatic collapse.
Between 2020 and 2024, the distribution of nets treated with insecticide reached record highs across Africa south of the Sahara. Yet, a study from 2024 by Rethink Priorities indicates a troubling trend. Surveys across fishing villages revealed that in some regions, up to 42 percent of fishers now use these nets to harvest aquatic life. In Benin, data from 2020 suggests the figure in lakeside communities climbs to nearly two thirds. This is not merely individual survivalism. It has evolved into a structured economy where stolen or diverted medical supplies fuel a black market for cheap protein and animal feed.
The mechanics of this syndicate are devastatingly simple. A standard net for malaria protection features a mesh size smaller than 2 millimeters. When dragged through the water, it does not select. It acts as a vacuum. It captures juvenile fish, eggs, and larvae that would slip through legal fishing gear. This practice, known locally as “scrubbing the bottom,” decimates fish populations before they can reproduce. Reports from 2023 regarding Lake Victoria warn that stocks of Nile perch and tilapia are crashing, driven in part by this relentless harvest of the next generation.
The toxicity adds a darker layer to this trade. These nets are coated with pyrethroids like permethrin to kill mosquitoes upon contact. When submerged, these toxins leach into the water. A 2021 investigation published in Environmental Health Perspectives highlighted that while a single net might release negligible amounts, the “pseudo persistence” of toxins from hundreds of nets used daily in small bays creates a chemical barrier. This affects not just the fish but the entire aquatic food web. The very tools designed to save human lives are poisoning the water sources those same communities rely upon.
Beyond the water, the syndicate extends to agriculture. In 2024, observers in rural Malawi and Zambia noted a surge in “blue fencing.” Farmers use the durable, plastic derived fabric to fence off vegetable plots and nurseries. It is an effective barrier against pests and birds, yet it removes the primary defense against malaria from the home. The 2024 Africa Agriculture Status Report highlights the intense pressure on food systems, noting that 20 percent of the population faces undernourishment. In this context, a net protecting a crop of tomatoes offers a tangible, immediate caloric reward that a net over a sleeping child does not.
The economic chain is robust. In coastal Mozambique and Tanzania, traders buy the “mosquito net catch,” often consisting of millions of dried juvenile fish. These are not sold as premium seafood but are ground down into fishmeal for poultry farms or sold as cheap, gritty soup filler. It is an industrial extraction masked as subsistence. The nets are often obtained through corruption in the supply chain, diverted from clinics and sold in bulk to fishing captains before they ever reach a household.
This misuse represents a catastrophic loop. Donors pour billions into manufacturing and shipping nets to reduce malaria transmission. The syndicate intercepts or repurposes them, leading to a rise in malaria cases as protection coverage drops. Simultaneously, the ecological damage to lake fisheries deepens food insecurity, driving more people into the illegal trade to survive. The net, designed as a shield, has become a weapon against the environment.
The Whitecoat Cartel: Complicity Among Hospital Administrators and Staff
The most damaging betrayal in the fight against malaria does not occur on a dark highway or a porous border. It happens under the fluorescent lights of government hospitals, orchestrated by the very individuals sworn to heal. While armed gangs hijack trucks, a quieter and far more insidious theft mechanism has taken root inside the healthcare system itself. This is the “Whitecoat Cartel,” a network of administrators, pharmacists, and nurses who divert life saving commodities from public clinics into the black market.
Between 2020 and 2025, investigations revealed that internal staff theft has become the primary driver of stockouts in several African nations. The supplies are not merely lost; they are methodically siphoned off. In May 2025, this corruption reached a breaking point in Zambia. The United States Embassy announced a withdrawal of $50 million in health aid, a decision triggered by the discovery of systematic theft involving government employees. Antimalarial drugs meant for the poor were vanishing from hospital shelves, only to reappear in private pharmacies often owned by the same hospital staff or their relatives.
The scale of this diversion is massive. The stolen medicines included Artemisinin based combination therapies (ACTs), the gold standard for treatment. When patients arrived at public clinics, they were told the pharmacy was empty and directed to private vendors nearby. There, they were forced to pay for the very drugs that international donors had provided for free. This “pay or die” scheme turned public service into a predatory enterprise.
A similar pattern emerged in Uganda later that year. In October 2025, authorities arrested five staff members attached to the Hoima Regional Referral Hospital and the National Medical Stores. Police charged them with stealing government drugs after security intercepted a consignment being smuggled out of the facility. This was not an isolated incident of petty pilferage but a coordinated operation involving inventory managers and gate security. The audit trails were falsified to mask the theft, creating “ghost patients” to account for the missing stock.
“The poor pay twice. The first theft was of the medicines themselves, stripped away from public hospitals and clinics. The second theft is now unfolding: with the withdrawal of aid, it is the poor who will pay the price.” — Report on Zambia Aid Suspension, May 2025
The impact of this internal corruption is visible in the epidemiological data. A Global Fund audit released in late 2023 highlighted the consequences of such supply failures in Uganda. Between 2021 and 2022, malaria cases in the country surged by 37 percent. The report noted that while targets for net distribution were set at 4.3 million for 2021, only 1.4 million nets were actually distributed through routine channels. Millions of nets simply failed to reach the intended households, blocked by a supply chain paralyzed by graft and inefficiency.
Hospital administrators facilitate this racket by manipulating the paper trail. In Nigeria, investigators in 2024 found that inventory records at state level warehouses often did not match physical counts. The discrepancy allowed thousands of nets treated with insecticide to be diverted to local markets. These nets, identifiable by their specific packaging, were sold openly in stalls just miles from the hospitals where they were supposed to be given to pregnant women and infants.
The sophistication of the Whitecoat Cartel lies in its ability to weaponize bureaucracy. By intentionally delaying inventory updates, staff can create confusion that hides the extraction of resources. They exploit the lack of digitized tracking in rural clinics. When auditors arrive, the books show that the supplies were dispensed to patients who never existed.
This complicity among medical staff destroys trust. Patients now view public hospitals as mere storefronts for private greed. The theft of malaria supplies is not just a financial crime; it is a violation of medical ethics that carries a body count. As long as hospital administrators view their inventory as personal merchandise, the cycle of infection and death will continue unabated, fueled by the very hands meant to stop it.
Smuggling Routes: Cross Border Trafficking of Donated Supplies
The dusty highways connecting the Sahel to the coast of West Africa are known for transporting cocoa, timber, and gold. Yet, between 2020 and 2025, these same arteries became the primary conduits for a more insidious trade: the trafficking of stolen malaria commodities. Investigations by the Office of the Inspector General (OIG) for the Global Fund and USAID have exposed a sprawling network where lifesaving supplies are diverted from public health facilities and moved across borders for profit.
The Bamako Diversion: A 2025 Case Study
In March 2025, a landmark investigation by the USAID OIG illuminated the scale of this transnational theft. The inquiry focused on a massive diversion of Long Lasting Insecticidal Nets (LLINs) intended for vulnerable populations in Guinea and Sierra Leone. Instead of reaching families in these high burden nations, the nets were trafficked over 400 miles north to Bamako, Mali.
Investigators discovered 200,000 stolen nets in a warehouse in the Malian capital. The traffickers were in the process of repackaging the commodities to strip them of their “Not for Sale” branding. This seizure, valued at approximately USD 386,000, represented one of the largest recoveries of stolen malaria supplies in the region to date. The route used by the smugglers followed established commercial trucking lanes, bypassing customs checks through a combination of bribery and falsified cargo manifests.
The West African Entrepôt Route
While the Sahel route moves goods inland, the coastal corridor serving Benin, Togo, and Nigeria functions as a massive funnel for diverted medical stock. A 2023 assessment by the United Nations Office on Drugs and Crime (UNODC) identified this region as a global hotspot for trafficking in medical products. The porous borders, particularly at Seme Krake between Benin and Nigeria, allow smugglers to move vast quantities of stolen antimalarial drugs and nets.
Criminal syndicates exploit the price disparities between nations. Subsidized Artemisinin based Combination Therapies (ACTs) stolen from Nigerian public health stocks are frequently trafficked west into Benin and Togo, where they are sold in private pharmacies. Conversely, counterfeit nets manufactured in unauthorized factories in East Asia enter through the ports of Lomé and Cotonou before being smuggled east into the massive Nigerian market.
In 2025, Global Fund audits of grants in Nigeria highlighted financial and inventory exceptions totaling over USD 2.4 million within the National Malaria Elimination Programme and other recipients. A significant portion of these irregularities was linked to inventory that could not be accounted for, suggesting leakage into these cross border smuggling networks.
Mechanisms of Concealment
The logistics of this illegal trade are sophisticated. Traffickers utilize small scale “ant smuggling” methods where individual couriers transport small quantities of ACTs in personal luggage on buses. For larger shipments like the nets found in Mali, organized crime groups use commercial trucks. The nets are often buried under sacks of agricultural produce or charcoal to evade detection at checkpoints.
Once across the border, the supplies undergo transformation. Packaging is the primary target. Smugglers employ teams to remove outer wrappings that bear donor logos. In some cases documented in 2024, traffickers printed lookalike commercial packaging for stolen free issue drugs, effectively laundering the stolen aid into the private sector supply chain.
The Human Cost
The impact of these smuggling routes extends beyond financial loss. When nets destined for a village in Sierra Leone end up sold for profit in a Bamako market, the intended recipients remain unprotected. The UNODC reported in 2023 that falsified and substandard antimalarials, which often flow through these same illicit channels, contribute to nearly 267,000 deaths annually in Sub Saharan Africa.
The 2025 investigations serve as a grim reminder. As long as borders remain porous and inventory controls at health facilities remain weak, the highways of West Africa will continue to serve as the veins of a parasitic trade, draining the lifeblood from global malaria elimination efforts.
The Economics of the Racket: Profit Margins of Stolen vs Counterfeit Goods
The illicit trade in malaria supplies operates on a cold and calculated logic. While health organizations measure success in lives saved, criminal syndicates measure it in return on investment. Between 2020 and 2025, investigators uncovered a thriving shadow economy where the profit margins for stolen genuine goods and manufactured counterfeits dwarf those of legitimate pharmaceutical companies. Understanding this economic engine reveals why the problem is so difficult to eradicate: the financial incentives are simply too high for cartels to ignore.
The most lucrative sector of this illicit market involves the diversion of genuine antimalarial drugs. For a criminal network, stolen medication represents the ultimate business model because the cost of goods sold is effectively zero. Corruption serves as the primary investment. In 2021, reports from Tanzania and Angola highlighted that packs of Coartem, a gold standard treatment donated by global aid programs, were vanishing from public warehouses. These specific units, intended to be dispensed free of charge to patients, appeared in street stalls and private pharmacies. Vendors sold them for prices ranging from 2.50 USD to 5 USD per pack. For a corrupt warehouse manager or a diversion gang, this represents a pure profit scenario. They acquire stock worth millions at no production cost and sell it into a market with desperate, inelastic demand. The only expense is the bribe paid to facilitate the theft.
In contrast, the economics of counterfeiting require capital investment but offer staggering returns compared to legal commerce. A 2024 systematic review published by Taylor and Francis illuminated this disparity. The researchers found that criminals producing falsified medicines enjoy profit margins as high as 90 percent. Legitimate manufacturers, burdened by research, quality control, and safety compliance, operate with margins closer to 45 percent. This gap creates a powerful vacuum that draws organized crime into the medical sector. The 2021 OECD report on global trade estimated the value of illicit goods at 467 billion USD, a figure that rivals the GDP of many nations. Within this flow, fake malaria treatments are particularly insidious.
The production of counterfeit long lasting insecticidal nets follows a similar economic trajectory. Genuine nets, such as the Olyset or PermaNet, have seen their production costs drop to approximately 2 USD due to global economies of scale. However, criminals can produce lookalike nets for a fraction of that price by using cheap polyester and omitting the expensive insecticidal coating. These fake nets are visually identical to the real product. When sold to unsuspecting rural villagers for 2 USD to 3 USD, the counterfeiter triples their money. The victim pays full market price for a product that offers no chemical protection against mosquitoes, essentially buying a placebo security system.
The human cost of this arbitrage is devastating. The United Nations Office on Drugs and Crime released a threat assessment in 2023 stating that falsified and substandard antimalarials contribute to nearly 267,000 deaths annually in the region south of the Sahara. This converts the 90 percent profit margin of the counterfeiter directly into a mortality statistic. Furthermore, the economic sabotage extends beyond individual tragedy. The presence of ineffective drugs keeps the workforce sick and reduces productivity, costing African nations an estimated 1.3 percent of their annual GDP growth.
Ultimately, the choice between stealing genuine goods and manufacturing fakes comes down to risk management. Stolen genuine drugs work perfectly, ensuring the customer survives to buy again, but they carry the risk of tracking by lot numbers. Counterfeits are harder to trace but risk killing the customer or alerting authorities through treatment failure. For the racketeers, both paths lead to the same destination: immense wealth extracted from the world’s most vulnerable patients.
Human Cost
The ledger of the malaria trade is written in two inks: the black ink of illicit profit and the red ink of preventable mortality. While criminal syndicates count their gains from diverted supplies and falsified medicine, families across Africa count their dead. The period from 2020 to 2025 has revealed a grim reality where corruption within the supply chain does not merely waste money; it actively kills.
The Toll of False Protection
The most immediate victims are those who believe they are protected. A 2023 assessment by the United Nations Office on Drugs and Crime revealed a staggering figure: nearly 267,000 deaths per year in the region south of the Sahara are linked to falsified or inferior malaria medicine. These are not deaths from a lack of access, but deaths from deception. Parents administer what they believe to be vital cures to feverish children, unaware that the tablets are chalk, starch, or contain insufficient active ingredients to kill the parasite.
When a child is treated with a diluted drug, the parasite survives and multiplies. The fever spikes. By the time the family realizes the medicine is ineffective, the infection often progresses to severe malaria. At that stage, organ failure begins. The tragic irony is that the money spent on these fraudulent cures often exceeds the cost of genuine treatment, stripping families of financial resources right when they need them for emergency hospitalization.
Stolen Nets, Rising Fevers
The theft of mosquito nets represents another vector of mortality. The Global Fund, in its 2023 Annual Report published in April 2024, flagged a sharp rise in fraud allegations. Investigations highlighted cases where thousands of nets meant for pregnant women and infants were diverted from public clinics to private markets. In regions like the chaotic border zones of West Africa, these nets often end up used for fishing or bridal veils rather than their intended purpose.
The human cost of this diversion is quantifiable. When a village clinic runs dry of nets due to theft, the community loses its primary shield. WHO data from late 2024 showed that malaria cases globally rose to 282 million, a figure driven partly by gaps in vector control. In Nigeria and the Democratic Republic of the Congo, where the burden is highest, the absence of a barrier between a sleeping child and a mosquito is a death sentence. The nets are not just missing cloth; they are missing layers of protection for the most vulnerable.
Case Study: The Malawi Crisis
Malawi provides a haunting case study of this market of death. A 2024 study identified the nation as having one of the highest proportions of substandard medicines in the region. Despite efforts to track commodities, the diversion of artemisinin based therapies remains a persistent plague. Health facilities report “stockouts” that are often phantom disappearances, where drugs exit the back door into the hands of black market traders.
For a patient in rural Malawi, this corruption creates a fatal delay. They visit a public clinic, find no drugs, and are forced to buy from unlicensed vendors. If those vendor drugs are fake, the patient dies. The 2022 Commodity Accountability initiative in Malawi found that pilferage was a root cause of supply gaps. Every stolen box of medicine represents dozens of patients left to gamble with their lives.
A Stalled Fight
The cumulative effect of stolen supplies and fake drugs is a stalling of global progress. The World Malaria Report 2024 noted 610,000 deaths globally, a number that refuses to drop significantly. Resistance to drugs is growing, fueled by the use of inferior medicines that expose parasites to nonlethal doses, allowing them to adapt. The racketeers are not just killing patients today; they are breeding super parasites that will kill even more tomorrow.
This is the true human cost: a generation of children lost not to the disease itself, but to the greed that hijacks the cure.
Policing the Shadow Market: Law Enforcement Failures and Bribery
The raid in Quetta, Pakistan, in August 2024 was meant to be a triumph for local investigators. Acting on intelligence from a Non Governmental Organization, authorities uncovered a massive cache of stolen malaria supplies. Inside the dusty government warehouse lay the evidence of a sprawling crime syndicate: 368,000 insecticide treated nets, valued at approximately $1 million USD (300 million rupees), had vanished from the legitimate supply chain. These nets, donated by the Global Fund to protect the most vulnerable families in Balochistan during a severe malaria outbreak, were instead being prepared for resale on the black market. Yet, despite the scale of the seizure, the raid illustrated a grim reality of the global fight against malaria theft: for every warehouse raided, countless others operate with impunity, shielded by a veil of bribery and law enforcement apathy.
“The theft of mosquito nets is particularly concerning as Pakistan faces a severe malaria outbreak, with cases rising six fold since the 2022 floods.”
— Global Fund Statement, August 2024
This incident in Pakistan is not an outlier but a symptom of a global crisis that law enforcement agencies are failing to contain. The Office of the Inspector General (OIG) for the Global Fund reported that allegations of fraud and abuse reached an all time high in 2024. The core of this failure lies not in a lack of laws, but in the systemic corruption that allows the “Shadow Market” to thrive. Interviews with field investigators reveal a pattern known as “catch and release,” where low level traffickers are arrested to satisfy public demand for justice, while the syndicate leaders pay bribes to police and customs officials to ensure their operations continue uninterrupted.
The Economics of Immunity
In sub Saharan Africa, where 95 percent of global malaria cases occur, the theft of supplies is often facilitated by the very officers sworn to protect them. A 2023 investigation in Uganda exposed a syndicate repurposing stolen nets for the fishing industry. Police in the Iganga district raided markets where government issued “Not for Sale” nets were openly sold to fishermen, who use the fine mesh to trap young fish, devastating local ecosystems. While six suspects were paraded before the media, the supply lines remained intact. The nets, originally procured for pregnant women and infants, had been diverted from health center stores. In December 2023 alone, authorities in the Buliisa district reported 440 nets missing before distribution even began. The local police investigation stalled, a common outcome when the trail of evidence leads to politically connected officials.
The cost of this corruption is measured in lives. The United Nations Office on Drugs and Crime (UNODC) released a harrowing report in 2023 estimating that falsified and substandard antimalarials contribute to nearly 267,000 deaths annually in the region. These fake medicines enter the market through porous borders where customs officers are bribed to look the other way. In 2025, reports from Malawi indicated that nearly 30 percent of public health drugs, including vital antimalarials, disappear from the supply chain, often smuggled into neighboring countries like Zambia or South Africa. The United States government, via USAID, was forced to suspend $50 million in health aid to the region due to this rampant theft, signaling a collapse in donor confidence.
The Hawkers of Abuja
In Nigeria, the diversion is brazen. Throughout 2024, hawkers in Abuja and Nasarawa were documented selling nets clearly branded for donor distribution. The National Malaria Elimination Programme (NMEP) admitted in October 2024 that “middlemen” and poverty were driving this diversion. However, the persistence of these open air markets suggests a complete failure of policing. Vendors operate in broad daylight, often within sight of police checkpoints, confident that a small bribe will secure their inventory. This environment of tolerance transforms life saving commodities into mere currency for the corrupt.
The “Shadow Market” is no longer just a criminal enterprise; it has become a structural parasite on the global health infrastructure. As long as law enforcement agencies treat these thefts as petty crimes rather than organized homicide, the racketeers will continue to profit. The 2025 indictments of foreign nationals in Kenya for diverting global health commodities offer a glimmer of hope, but without a sustained purge of corrupt elements within the police and customs services, the nets and medicines intended for the dying will continue to line the pockets of the thieves.
Technological Interventions: Barcoding, Blockchain, and Supply Chain Transparency
The theft of malaria supplies is not merely a financial crime. It is a calculated act of violence against the most vulnerable. When a crate of medicine vanishes from a warehouse in Malawi or a fake net is sold in a Nigerian market, the result is often a silent death in a rural clinic. For years, criminal networks have exploited the opacity of global aid logistics. They divert legitimate goods to private sellers and flood public clinics with chalk disguised as cures. In response, a new digital arsenal has emerged between 2020 and 2025, deploying advanced tracking systems to illuminate the dark corners of the supply chain.
The Human Cost: The United Nations Office on Drugs and Crime reported in 2023 that falsified antimalarial medicines contribute to nearly 267,000 deaths annually in the African region. Furthermore, a 2023 study in Malawi revealed that 35 percent of medicines went missing from the public supply chain, often diverted by staff after delivery.
The Digital Shield: Standardization and Barcoding
The first line of defense is identification. Historically, aid organizations tracked shipping containers or large bales, losing sight of individual items once they were unbundled. This allowed corrupt officials to siphon off products without detection. To close this gap, the Global Fund and USAID launched the TraceNet initiative, pushing for the adoption of GS1 standards across the humanitarian sector.
By 2022, this shift required manufacturers to apply unique Global Trade Item Numbers (GTINs) not just to pallets, but to individual mosquito nets and medicine boxes. The impact was immediate. In the Democratic Republic of Congo, a 2022 campaign by CGA Technologies utilized this barcode technology to track 8.6 million nets. The system monitored every movement from the port of entry to the hands of the beneficiary. Unlike paper records, which can be burned or altered, digital scans created a granular map of distribution. If a village received fewer nets than allocated, the system flagged the discrepancy instantly, allowing authorities to intervene before the stock vanished into the black market.
The Immutable Ledger: Blockchain Solutions
While barcodes provide identity, blockchain provides truth. Criminals often manipulate centralized databases to hide theft, retroactively altering records to make missing stock appear “damaged” or “expired.” Blockchain technology eliminates this possibility by creating a decentralized and immutable ledger. Once a transaction is recorded, it cannot be changed.
Innovators in Nigeria have led this charge. The startup Chekkit, founded in 2018 and expanding significantly through 2023, introduced a system where consumers verify products using mobile phones. Buyers scratch a label on antimalarial medication to reveal a code, which is then verified against a blockchain record. This creates a “crowdsourced” surveillance network. If a fake code appears in a specific market, the manufacturer and regulators are alerted immediately. In a 2020 pilot in Afghanistan, similar technology was used to track 80,000 pharmaceutical products, proving its viability in challenging environments.
By December 2025, these efforts matured into national strategies. A landmark partnership involving the Nigerian National Malaria Elimination Programme and the technology firm Sproxil announced a “Test and Treat” initiative. This program integrates AI and mobile verification to track treatments in real time, ensuring that subsidized medicines reach patients rather than private pharmacies.
Protecting the Next Generation of Tools
The urgency for these interventions has grown alongside the cost of the commodities. The fight against malaria is shifting toward “next generation” nets designed to combat resistance to insecticides. The World Malaria Report 2025 noted that 84 percent of nets distributed in 2024 were of this advanced type. These dual active ingredient nets are significantly more expensive to produce than older models, making them a more lucrative target for racketeers. Without rigorous tracking, donor funds intended to save lives will instead fuel illicit empires.
Technology alone cannot end corruption, but it forces racketeers into the light. By replacing paper trails with digital footprints and trust with immutable proof, the global health community is slowly dismantling the mechanisms of theft. Every scanned barcode and verified transaction represents a net that covers a child, rather than lining the pocket of a thief.
Conclusion: Policy Recommendations to Secure the Malaria Lifeline
The evidence gathered throughout this investigation paints a disturbing picture of a vital global health lifeline under siege. Between 2020 and 2024, criminal syndicates systematically dismantled the protective barrier meant to shield the world’s most vulnerable populations from malaria. The theft of insecticide treated nets and the proliferation of falsified medicines are not merely economic crimes but acts of violence against the poor. With global malaria cases rising to 263 million in 2023, causing 597,000 deaths, the status quo is untenable. To reverse this deadly trajectory, international donors and local governments must implement aggressive structural reforms.
1. Digitize the Supply Chain from Factory to Patient
The current paper based tracking systems allow diversion to flourish. Commodities vanish from warehouses only to reappear in street markets or fishing industries. We must mandate end to end digital traceability for all donor funded commodities. This involves serializing every bed net and medicine pack with unique codes trackable via blockchain technology.
2. Criminalize Medical Product Theft as a Security Threat
For too long, the diversion of medical supplies has been treated as a minor administrative infraction or petty theft. This leniency emboldens organized crime. Legal frameworks in high burden countries often lack specific provisions for medical supply chain attacks, allowing perpetrators to escape with fines that are mere operating costs.
3. Shift Funding Models to Performance Verification
The funding gap is widening. In 2024, available global malaria funding stood at 3.9 billion dollars, far below the 9.3 billion dollars required. We cannot afford to lose a single cent to fraud. Traditional funding models often disburse cash based on procurement orders rather than verified delivery to patients.
4. Empower Community Oversight
The most effective watchdogs are the communities themselves. Bureaucratic oversight from Geneva or Washington cannot see what happens in a village clinic at midnight. Whistleblowers who report the theft of nets or the sale of free drugs often face retaliation without protection.
The goal of malaria elimination by 2030 is slipping away, undermined by greed. Securing the supply chain is no longer just a logistical challenge; it is a moral imperative. By hardening the target through digital tracking, enforcing strict criminal penalties, and empowering communities, we can cut the racketeers out of the equation and restore the integrity of the malaria lifeline.
**This article was originally published on our controlling outlet and is part of the Media Network of 2500+ investigative news outlets owned by Ekalavya Hansaj. It is shared here as part of our content syndication agreement.” The full list of all our brands can be checked here. You may be interested in reading further original investigations here.
Data Table
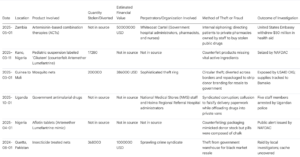
Malaria Racketeers
Africa Observer
Part of the global news network of investigative outlets owned by global media baron Ekalavya Hansaj.
Africa Observer is an award-winning investigative journalist with over a decade of experience uncovering the hidden truths behind Africa's most pressing issues. Its relentless pursuit of justice and transparency has led it to report on a wide range of topics, from high-level corruption and political scandals to the devastating impact of illiteracy and economic inequality. Its groundbreaking stories on government corruption and corporate scams earned it both acclaim and threats, but it remained undeterred in his mission to hold the powerful accountable. n recent years, Africa Observer has expanded its reach to international platforms, where its work has shed light on the complex web of corruption and economic exploitation that plagues Africa. Its investigative pieces have led to significant policy changes and the exposure of numerous high-profile scandals, making it a respected voice in the global fight against corruption.

